Physical Therapy Videos - Knee
What Is It?
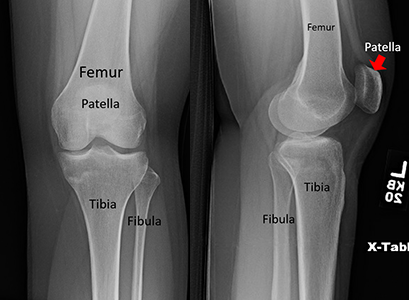
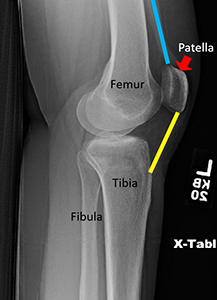
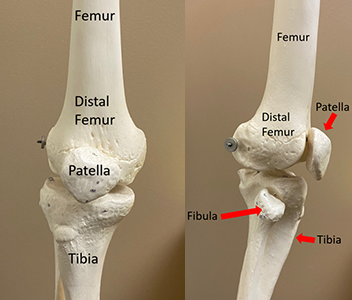
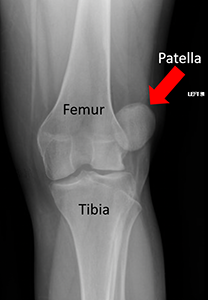
The knee has three bones: the thighbone (femur), the lower leg bone (tibia), and the kneecap (patella). Your kneecap is in the middle of a big tendon that connects your front thigh muscles to your lower leg bone. This helps your knee bend. The bottom of your kneecap and the top of a groove on your thighbone are covered with thick cartilage. This lets bones move easily over each other. If this cartilage gets damaged, it can lead to arthritis.
How It Happens
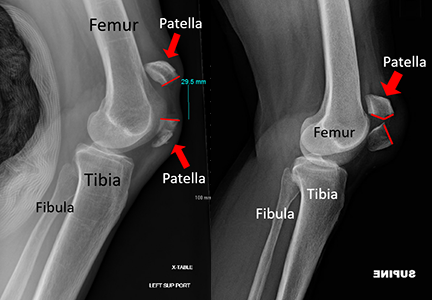
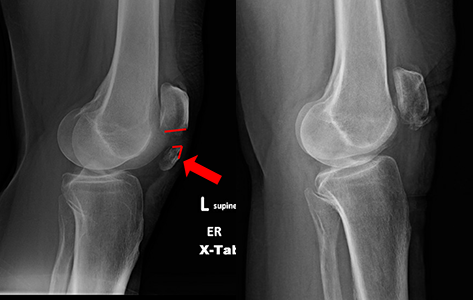
Kneecap fractures are quite common. They can happen after a hard hit to your kneecap, often during a fall. They can also happen if your thigh muscles tense up very strongly, but this is less common.
First Steps
If you break your kneecap, your knee will swell up and you might not be able to straighten your leg. You probably won't be able to walk because of the pain and trouble using your leg. Doctors at the emergency room or urgent care will take x-rays to see if your kneecap is broken. If the skin over your kneecap looks okay, you may be treated with a leg brace and go home. You'll need to see a doctor soon after for more treatment.
Treatment
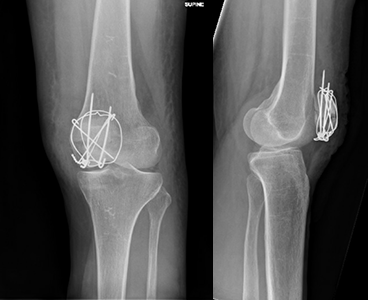
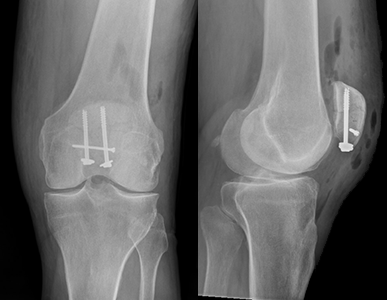
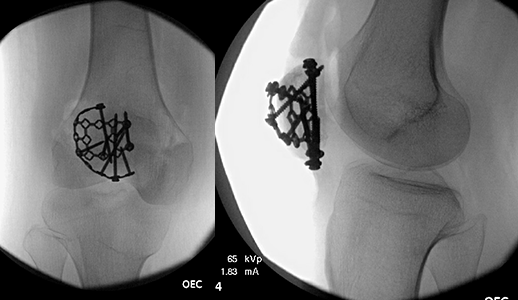
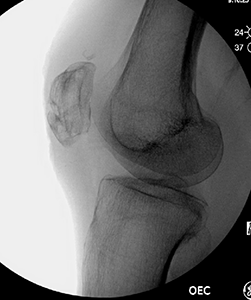
Treatment depends on whether the bone pieces are touching and if your leg can be straightened. If the pieces are pulled apart, you'll likely need surgery to put them back together. If there's just a crack in the kneecap and the bones aren't pulled apart, you may not need surgery. Instead, you'll likely be treated with a brace and have limits on bending and weight bearing. Surgery for a broken kneecap can be done in many ways. The main goal is to reconnect the bones. Common ways to fix a kneecap are with wires, plates, sutures, or a combination of these.
Recovery
After surgery, you'll likely be in a brace that limits how much you can bend your knee. You might be able to walk with your leg held straight by the brace. Your doctor will tell you if you can put weight on your leg and how much you can move your knee. It's important to follow your surgeon's advice. You might need physical therapy after surgery to help you recover.
Long Term
After healing, most people can go back to their normal activities. This can take several months. Your kneecap has a thick layer of cartilage, which can be injured during the break. This may lead to arthritis in your knee joint. Arthritis can cause pain and stiffness. Your knee might also become stiff after it has healed. You may not be able to bend or straighten it as much as before. Sometimes you need more treatment to regain motion in your knee. If the hardware used to fix your kneecap bothers you, it might need to be removed after your bone heals. This requires another surgery. Sometimes the wires or screws can become loose and need to be taken out. If your kneecap fracture doesn't heal, the bone pieces may pull away from each other. If this happens, you'll likely need more surgery to reconnect the bones. Other problems that can happen are issues with wound healing or blood clots. These aren't common, but they do happen. It's important to follow your surgeon's advice to try to prevent these problems.
Physical Therapy Videos - Knee
More Information
---
Christopher Domes, MD
Edited by the OTA Patient Education Committee
All x-rays and pictures taken from the personal collection of Dr. Domes