Physical Therapy Videos - Femur
What Is It?
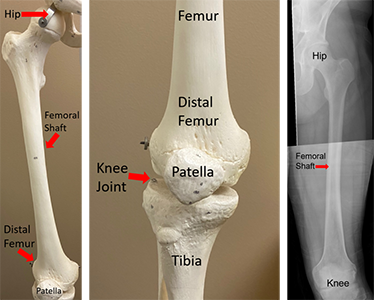
The thigh bone, or femur, is the biggest bone in your body. It is the only bone in the top part of your leg and is surrounded by thigh muscles. The middle part of your thigh bone is called the femoral shaft. The top of your femur connects to your hip, and the bottom connects to your lower leg at the knee.
How It Happens
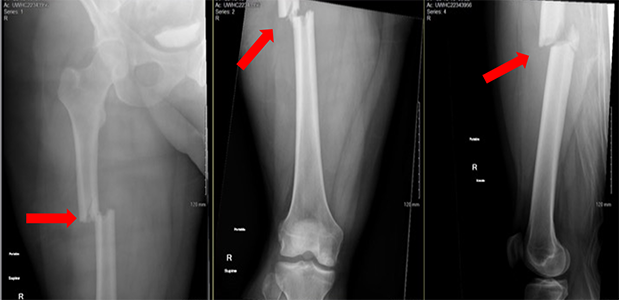
A lot of force is needed to break your femur. This can happen in a car crash, falling from high up, or during fast activities like skiing or biking. People with broken femurs often have other injuries too. Some of these injuries can be very serious or even life-threatening.
First Steps
Breaking your femur is very painful and makes your leg look bent or floppy. You can't walk on it, so you'll need an ambulance. Sometimes, paramedics or first responders will put a temporary brace, straps, or pillows around your leg to keep it still and hurt less. At the hospital, doctors will check you all over for other injuries and take x-rays. They might also need a CT scan to look for more injuries.
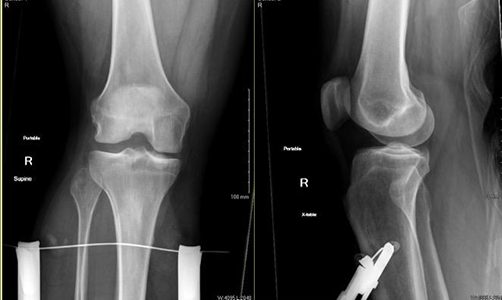
Femur breaks almost always need surgery. If doctors can't do surgery right away, they might put a "traction pin" in your leg to help keep the bone lined up. They put the pin in at your bedside with numbing medicine.
Treatment
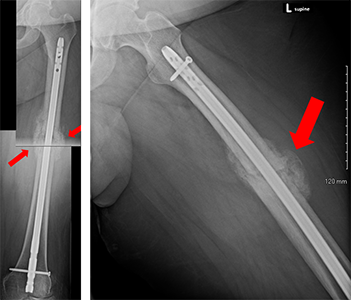
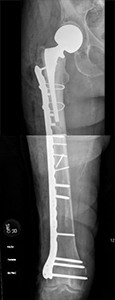
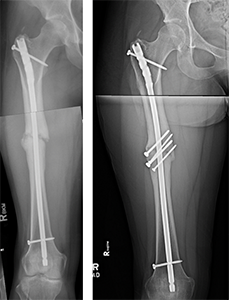
The most common way to fix your broken femur is to put a metal rod inside your bone. The rod and screws hold the broken bone in place. You might be allowed to put weight on your leg right after surgery, but that depends on your surgeon.
Other treatments include using a metal plate and screws or an external fixator to hold the bone in place. These options are used if a rod can't be put inside your bone.
Recovery
You'll probably stay in the hospital for a few days after surgery. Nurses and therapists will help you start walking again. You might need crutches or a walker for a while, and you may need to go to a rehab or nursing facility. It's important to do exercises to keep your hip and thigh muscles strong and avoid stiffness. You'll see your surgeon a few times for check-ups and x-rays to make sure your bone is healing.
Long Term
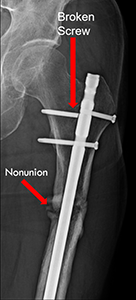
Usually, femur breaks heal after surgery. It takes about three months or more for the bone to fully heal. If it doesn't heal, you might need more surgery to help the bone heal. Once your femur is healed, you can usually go back to doing the activities you did before your injury. Some people might have stiffness or soreness, but these problems usually get better over time.
Physical Therapy Videos - Femur
More Information
---
Paul S. Whiting, MD
Edited by the OTA Patient Education Committee and Justin Haller, MD (section lead)
All x-rays and pictures taken from the personal collection of Dr. Whiting and Christopher Domes, MD