What Is It?
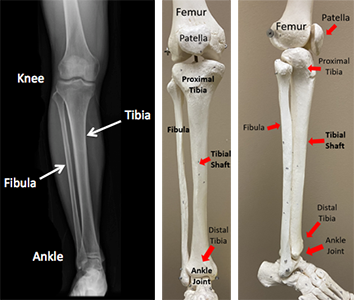
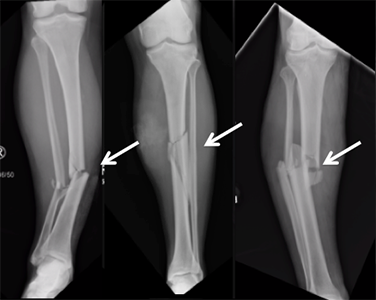
A broken lower leg bone happens when the tibia, one of the two bones in your lower leg,breaks. The tibia is the big bone between your knee and ankle, and it helps support your leg. The fibula, the other bone, adds stability to your knee and ankle. When the tibia breaks, the fibula might break too. Your leg has groups of muscles that do the same movements. The front muscles are smaller than the back ones, and you can feel the tibia bone under your skin. When the tibia breaks, it can poke through your skin, causing an "open" or "compound" fracture.
How It Happens
Broken lower leg bones can happen from twisting injuries, like in sports, or direct hits, like in car accidents. These fractures are common and often need surgery.
First Steps
If you break your lower leg bone, it will be painful, and you might not be able to move or stand on it. You'll need to go to the emergency room. Doctors will take x-rays of your leg and put your leg in a splint to reduce pain. Sometimes, you'll need to stay in the hospital for more treatment or surgery.
Treatment
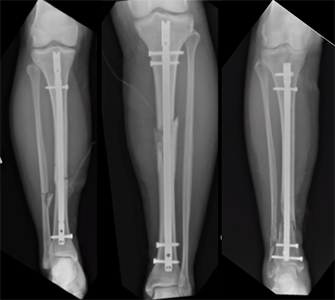
Most of the time, you'll need surgery to fix a broken lower leg bone. A "rod" or "nail" is put inside your tibia to help it heal. Sometimes a plate and screws is used if the break is near your knee or ankle. You'll get antibiotics before surgery to avoid infections.
Recovery
After surgery, you might be able to walk right away, or you might need crutches or a walker for a while. Physical therapy can help you get stronger and heal. You might get a blood thinner to prevent blood clots. You'll need to see your surgeon a few weeks after surgery and follow their instructions. If you broke other bones then just the tibia, recovery may be slower.
Long Term
You may need a walker or crutches for some time after surgery. Physical therapy can help you get back to normal walking and strengthen your muscles. Sometimes there are complications, like blood clots, infections, or problems with walking. If you have these problems, you might need more treatment or surgery. Sometimes the metal rods/plates put in during surgery need to be taken out.
More Information
---
Lucas S. Marchand, MD
Edited by the OTA Patient Education Committee and Justin Haller, MD (section lead)
All x-rays and pictures taken from the personal collection of Dr. Marchand and Christopher Domes, MD